The diagnostics of neurology is changing. With the emergence of a digital systemic foundation of healthcare, the capacity to consolidate various forms of clinical data has grown vital. Although Picture Archiving and Communication Systems (PACS) have long been applied to radiology, the neurophysiological information, specifically in the form of electroencephalography (EEG), has always lived in isolated systems.
Such discontinuity generates ineffectiveness in diagnosis, time lapses in clinical decision-making, and the difficulty of multidisciplinary collaboration. The interpretation of EEG signals and imaging data (like MRI or CT scans) is usually required by neurologists, radiologists, and critical care teams, but these data can hardly be presented within a single workflow.
EEG should be incorporated with PACS to bridge this gap. Allowing the access to the imaging and neurophysiological data in a centralized manner, healthcare providers will be able to gain a better understanding of the brain functioning and structure--which will eventually enhance the precision of the diagnosis and patient outcomes.
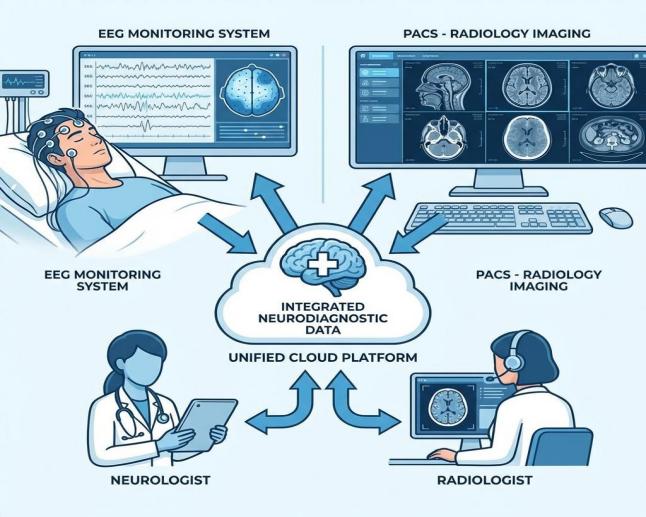
• Integrates Functional (eeg) And Structural (mri/ct) Data Systems.
• Facilitates Neurological Diagnosis.
• Enhances Teamwork Between Neurology, Radiology, And The Icu.
• Provides Remote Access And Tele-neurology Throughcloud Pacs Platforms
• Improves Clinical Performance In Multi-location Health Care Settings.
Question: What is EEG-PACS integration, and what is the significance of this feature in the context of neurological diagnostics?
Answer:
EEG-PACS integration can be defined as a mechanism that involves the storage, administration, and access to electroencephalography (EEG) data (usually in the form of DICOM waveforms) within a PACS environment, along with imaging examinations like MRI and CT scans. This enables clinicians to study the workings of the brain and the anatomical structures as a single system, enhancing diagnostic accuracy, clinical efficacy, and multidisciplinary teamwork, specifically in epilepsy monitoring, intensive care, and treating neurodegenerative diseases.
EEG and PACS have very different but complementary functions in the diagnosis of the nervous system.
EEG records electrical activity within the brain and it is used to reveal functional abnormalities in the brain, such as seizures, encephalopathy and sleep disorders. It produces continuous time-series data of waveforms that represents the activity of the neurons in various parts of the brain.
PACS, conversely, is made to handle medical imaging records, such as MRI, CT, and X-ray imaging. It facilitates storage, retrieval, and distribution of DICOM images based on a healthcare imaging infrastructure.
Each system can be used separately to offer useful yet incomplete information. EEG describes the working of the brain, whereas imaging demonstrates the structural defects. The combination of both allows clinicians to correlate the function with anatomy, which is a vital need in contemporary neurological diagnostics.
 - Presented by PostDICOM.jpg)
The main problem of the EEG-PACS integration is the fundamental difference between the data of the waveforms and the data of the imaging.
| Aspect | EEG Data | Imaging Data (PACS) |
| Data Type | Time-series waveform | Pixel-based images |
| Format | Proprietary / DICOM waveform | DICOM image |
| Clinical Insight | Functional brain activity | Structural anatomy |
| Nature | Continuous & dynamic | Static slices |
| Interpretation | Temporal analysis | Visual interpretation |
EEG data is time-dependent and continuous as opposed to imaging. This must involve the use of PACS systems that include specialized standards like DICOM waveform object and advanced visualization systems that can process time-series data.
Technically, the EEG connectivity with the PACS means that EEG data has to be transformed into common formats and has to be channeled through an interoperable infrastructure.
 - Presented by PostDICOM.jpg)
The diagnosis of epilepsy should be conducted with accurate correlations between the activity of seizures (EEG) and structural defects (MRI/CT). Both forms of analysis can be done at the same time, which greatly enhances the accuracy of the diagnosis and the treatment plan, as well as reduces the time taken by clinicians.
Continuous EEG monitoring is critical in the ICU as it helps in the identification of brain dysfunction and non-convulsive seizures. PACS integration allows remote specialists to access EEG in real-time with imaging to intervene faster.
EEG, in conjunction with other physiological data, is used in sleep studies. Integration facilitates central storage and simplifies longitudinal monitoring of the status of patients.
Structural analysis and functional analysis are needed in such conditions as Alzheimer's and Parkinson diseases. EEG-PACS integration facilitates the overall and continuous evaluation of the patient.
Not all the facilities need instant EEG-PACS integration. Nonetheless, it is necessary in certain situations:
• Neurological Or Epilepsy-related Hospitals.
• Icus With Constant Eeg Requirements.
• Multi-location Networks Of Healthcare.
• Remote Diagnostic Or Tele-neurology.
• Minor Clinics Without Eeg Systems.
• Low Neurological Case Volume Facilities.
The layer of decision assists the healthcare providers to coordinate the investment and clinical requirements.
Cloud PACS does not only enable- it forms the basis on which EEG integration becomes scalable and feasible.
• Single Access At Multiple Locations.provides The Ability To Access Eeg And Imaging Data Anywhere By The Neurologist.
• High-volume Data Scalability.constant Eeg Produces Massive Amounts Of Data- Cloud Systems Are Efficient With This.
• Tele-neurology Enablement.remote Diagnosis And Specialist Consultation.
• Clinical System Interoperability.integrates Seamlessly With Ehr, Ris, And Integration Engines.
• Reduced It Burden.removes The On-premise Infrastructure Management.
 - Presented by PostDICOM.jpg)
The EEG integration is far more effective in the modern healthcare setting when it is developed on the basis of cloud-based PACS architecture.
| Feature | EEG Standalone Systems | EEG Integrated with PACS |
| Data Access | Isolated systems | Unified access |
| Clinical Workflow | Fragmented | Streamlined |
| Collaboration | Limited | Multidisciplinary |
| Diagnosis Speed | Slower | Faster |
| Remote Access | Restricted | Enabled |
| Scalability | Limited | High (cloud-based) |
| Benefit | Impact |
| Unified Workflow | Eliminates system switching |
| Improved Diagnosis | Combines functional + structural insights |
| Faster Decision-Making | Real-time access to all data |
| Enhanced Collaboration | Supports cross-specialty teams |
| Remote Accessibility | Enables telemedicine |
EEG-PACS integration has a number of challenges despite the benefits it possesses.
• The Handling Of Large Quantities Of Continuous Reporting Eeg Data.
• Making Sure That It Is Compatible With Dicom Waveform Standards.
• Incorporating Old Eeg Systems.
• Training Clinical Staff
• Realigning The Workflows In The Departments.
• Long Recordings Optimization.
• Effective Indexing And Retrieval.
Multimodal integration is the future of neurological diagnostics.
• Computer-aided Eeg Interpretation.
• Eeg-mr/ct Fusion Co-diagnostic Techniques.
• Live Cloud-based Brain Surgery.
• Interconnection With Wearable Neurotechnology.
These innovations will reshape the nature of diagnosis and treatment of neurological diseases by clinicians.
Combining EEG and PACS is a significant development in the diagnostics of neurology. The combination of functional brain activity and structural imaging can help healthcare professionals to learn more about the condition of patients.
This integration is becoming a strategic requirement in the current healthcare settings, especially those that are utilizing cloud infrastructure. It enhances the accuracy of diagnosis, fastens clinical processes, and supports scalable and collaborative models of care.
A DICOM waveform is a standard format whereby one can store and retrieve EEG signals in PACS systems.
Yes, it is possible to save EEG in PACS in the form of DICOM waveforms.
It allows conduction of a unified analysis of both brain function and structure, enhancing diagnostic accuracy.
Yes, especially in tele-neurology and remote diagnostics.
With DICOM extensions of waveforms and compatible viewers, modern PACS systems are able to support EEG.
EEG is used to measure the activity of the brain, whereas EMG is used to measure muscle activity. They both may be saved as waveform data; however, they have different diagnostic applications.
|
Cloud PACS and Online DICOM ViewerUpload DICOM images and clinical documents to PostDICOM servers. Store, view, collaborate, and share your medical imaging files. |