Healthcare finally gets this. You expect access to your records, a real explanation of what's wrong, and a say in what happens next. The U.S. Office of the National Coordinator for Health IT pushed electronic health records into most hospitals. That helped. But one piece stayed locked away: your imaging.
Your MRI. Your CT scan. The X-ray that showed something concerning.Radiology drives decisions in cancer treatment, heart disease, brain disorders, broken bones, emergency rooms—pretty much everything.
The systems were built for doctors and IT departments, though. Not you. So you ended up on the outside of the most important visual evidence about your own body.
Web-based DICOM viewers are fixing that gap.
These aren't just picture viewers. They're cloud platforms that let your oncologist in another state pull up your scan in seconds, let your local doctor skip the CD-burning nightmare, and let you log in from your couch and actually see what the radiologist saw. Because it's your scan and you should be able to look at it whenever you want. They're becoming the infrastructure that makes patient-centered care actually work instead of just being something hospitals say in brochures.
• Web-based Dicom Viewers Get Rid Of The Old Access Problems You'd Run Into With Workstation-dependent Pacs Systems.
• Zero-footprint Architecture Lets You View Imaging Securely Right In A Browser — No Local Installation Needed.
• Real-time Visualization Helps Patients Understand What They're Looking At, Which Makes Shared Decision-making Way More Effective.
• Security Frameworks At The Enterprise Level Keep You Compliant With Hipaa And Gdpr While Opening Up Access To More People.
• Cloud-native Deployment Improves Scalability And Cuts Down On Infrastructure Complexity At The Same Time.
• Modernizing Imaging Supports Telemedicine, Lets Multiple Sites Work Together And Long-term Transformation.
Old imaging systems were built around PACS servers sitting in hospital basements. PACS — that's Picture Archiving and Communication Systems, per the Radiological Society of North America — got designed mostly for storage and for radiologists to read studies on workstations.
If you wanted to see your own scan, you had to be at the hospital using their specific viewer software. When patients asked for copies, they'd get a CD with DICOM files (that format comes from the National Electrical Manufacturers Association standard) or maybe just flat images printed alongside the report.
That setup caused problems.
Technical ones, mostly. A lot of people couldn't even open DICOM files, and these days most laptops don't have CD drives anymore, so the disk just sits there gathering dust or propping up a coffee mug. Communication was weird too — doctors would describe what they saw instead of just showing you the image and walking through it together, which made everything feel abstract and secondhand. If two hospitals needed to share a scan, someone had to physically mail a disc or set up some secure tunnel between networks, which took forever and usually required at least three IT tickets. Telemedicine kind of struggled with imaging even as telehealth exploded globally (the World Health Organization has been pushing digital health for years now).
None of this was because hospitals were doing clinical work badly. It's that the infrastructure itself had limits baked in from the start, limits that made sense when everything happened in one building but collapsed the moment care started happening anywhere else. Now that care is spreading out — you've got in-person visits, remote consults, specialists collaborating across cities — imaging needs to move around as easily as any other part of the medical record.
Which it doesn't.
A web-based DICOM viewer today doesn't need anything installed on your machine. Zero footprint. You log in through the browser, get authenticated with encryption and identity checks, and you're in.
The better platforms use DICOMweb standards — WADO-RS, QIDO-RS, STOW-RS — all straight from the official DICOM documentation, which means imaging archives can talk securely to web apps without reinventing the protocol every time since these are RESTful services built for exactly that.
Instead of downloading entire datasets to a workstation, the images get streamed in pieces or rendered on the server. Fast. Secure too.
Enterprise setups add role-based access, multi-factor authentication, audit logs that track every interaction, and encrypted storage, then connect to EHR systems and identity providers through APIs so referrals and clinical workflows stay intact without breaking at the handoff points.
This isn't just an interface upgrade — the architecture itself is different, and imaging used to live in a department, locked to specific machines, but now it's a distributed digital resource that travels with the patient across devices, across facilities, across care settings, though only if you have the right credentials to begin with.
The biggest shift happens right where patients and doctors meet.
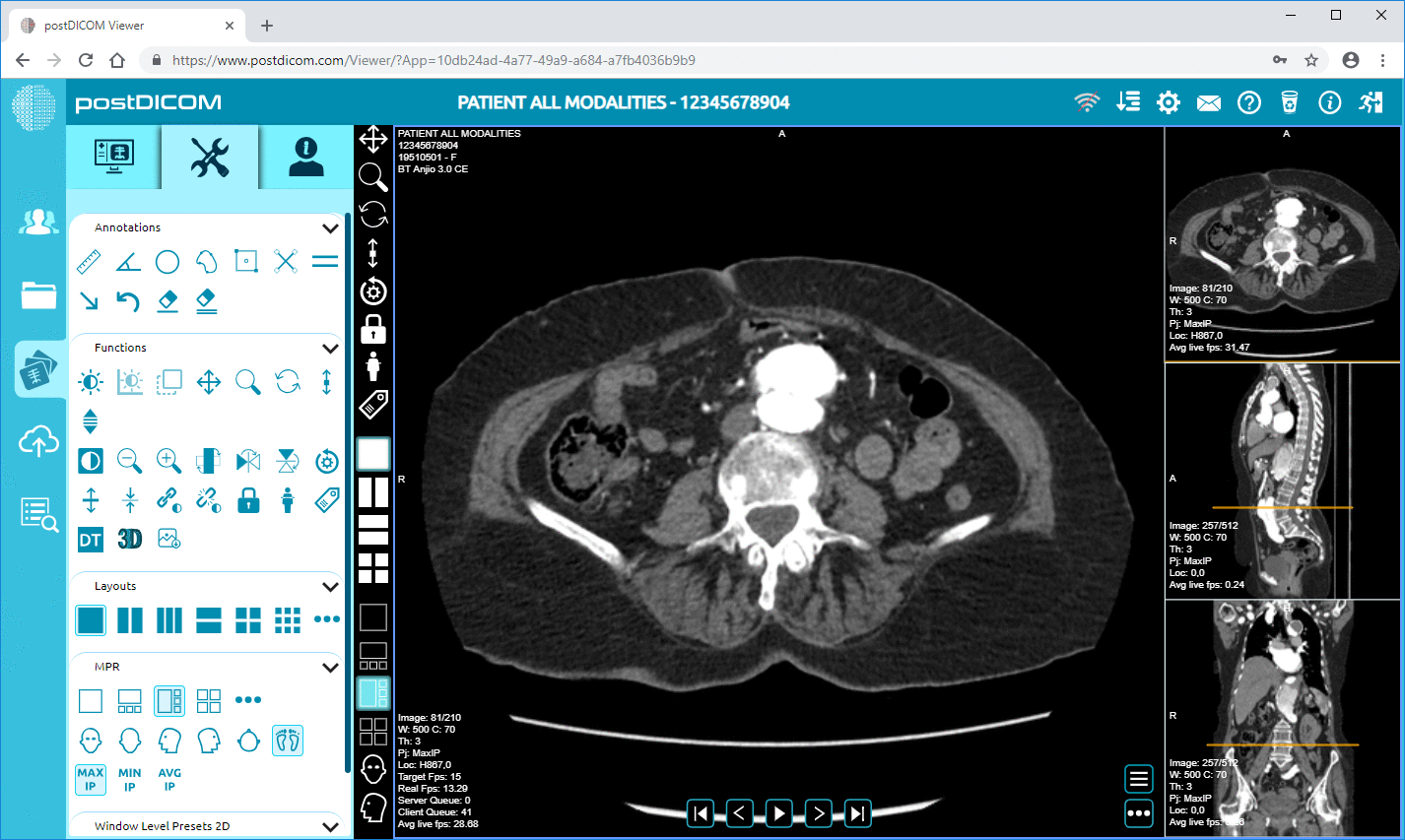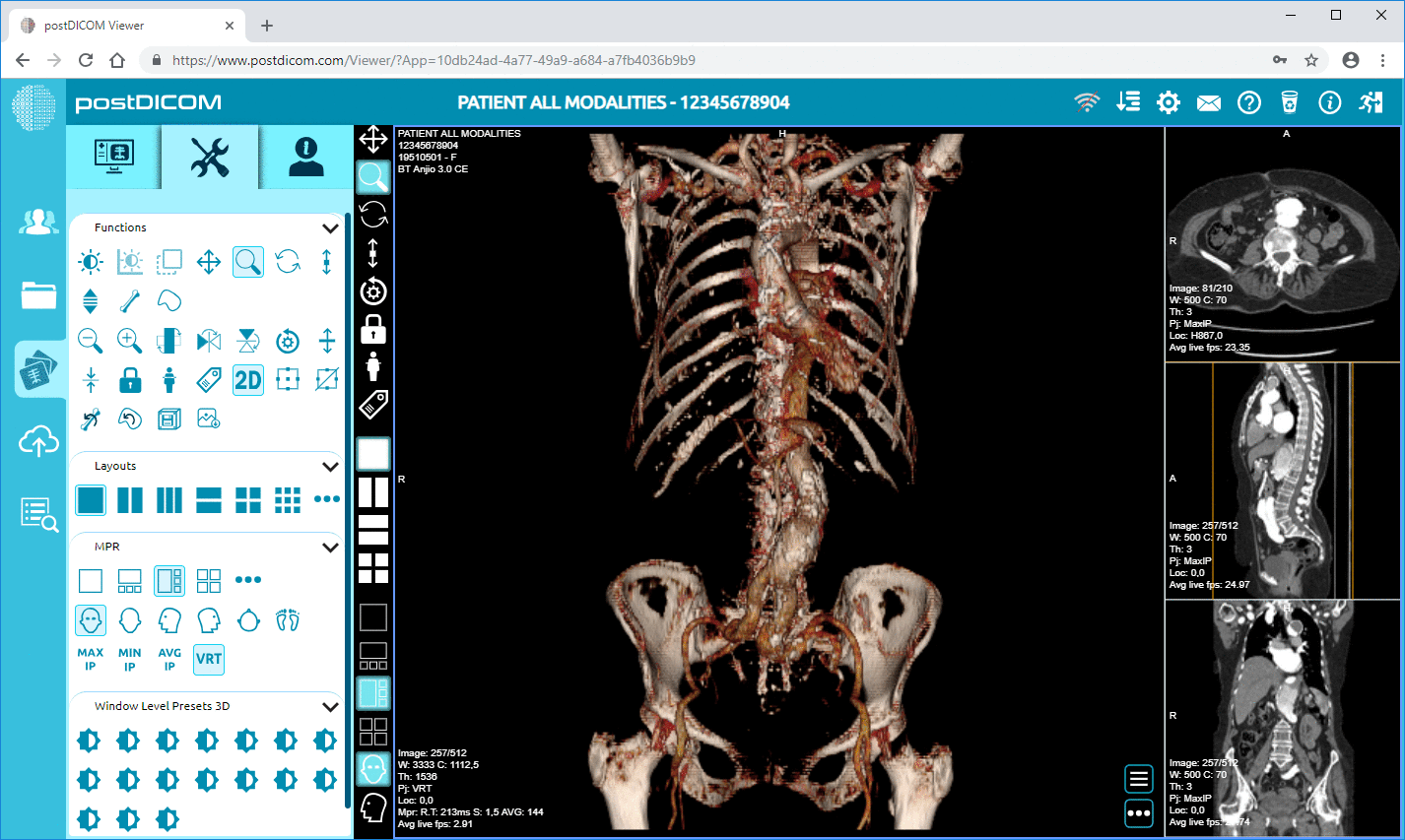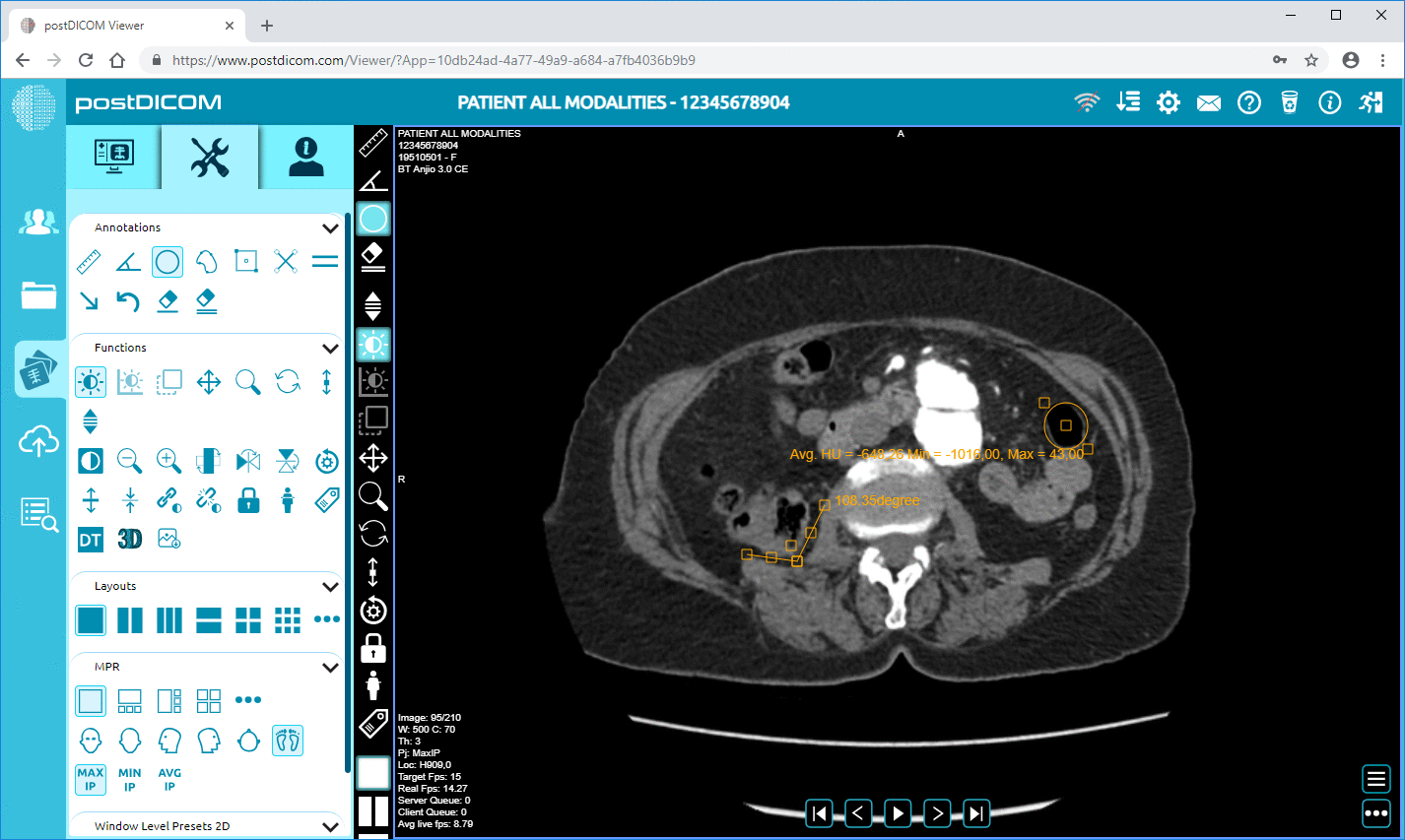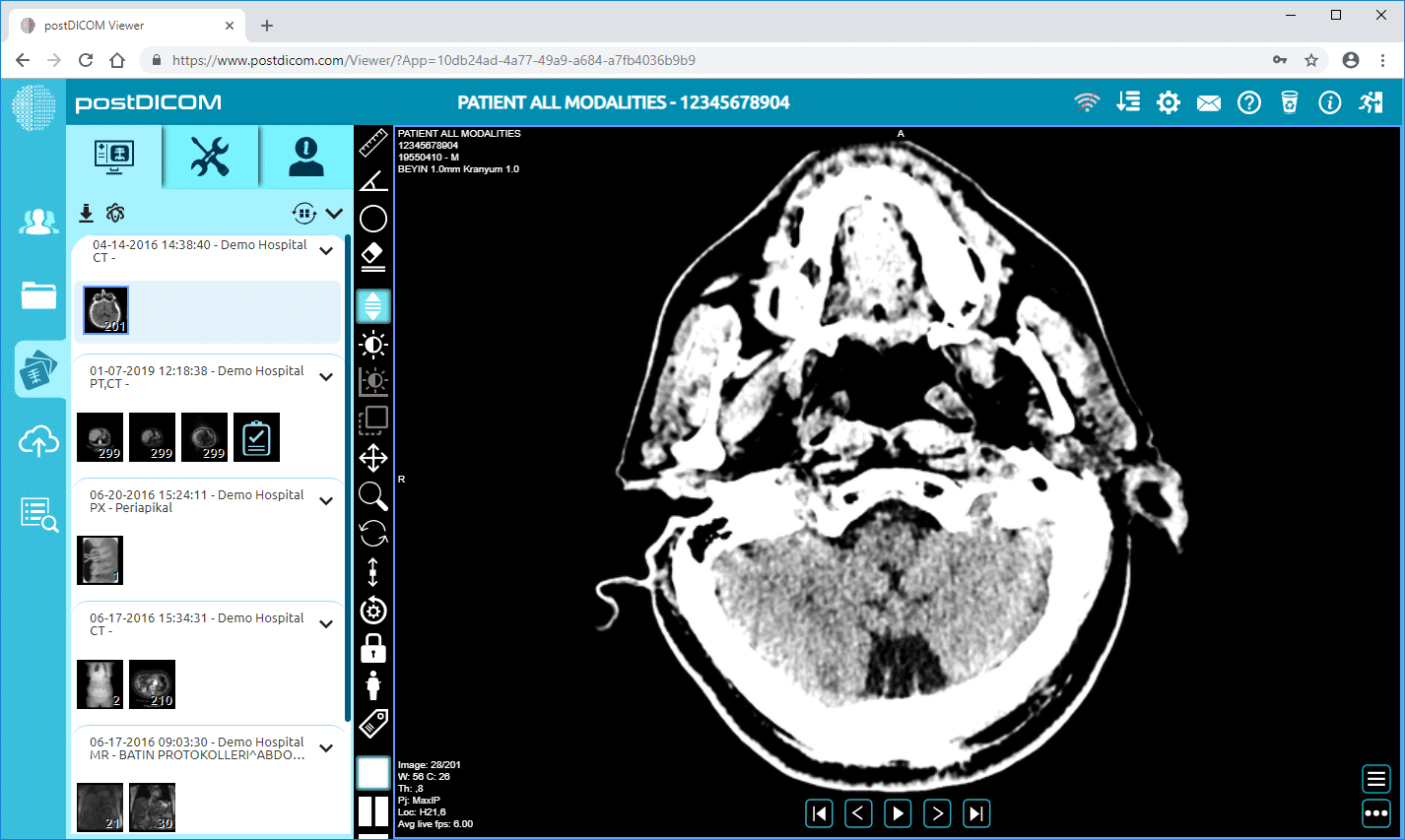
Cancer follow-ups, for instance. A doctor pulls up the CT scans — before treatment, after — right there on the screen. They can measure how much the tumor shrank. Live. While you're sitting there. It's not just hearing "you improved 40 percent." You're seeing the actual difference in your body, and that kind of visual proof does something for people emotionally; they stick with their treatment plans better because of it, sometimes without even being told why.
For orthopedic surgery, surgeons can spin a 3D model of your fracture around during the appointment, showing you exactly where the break is, where they're going to put the screws or plates, and why the procedure even makes sense in the first place. Consent stops being this abstract thing you sign off on. It becomes grounded — you both looked at the same image and talked through it.
Stroke cases over telemedicine work similarly, except a neurologist can walk a patient's family through brain scans during a video call, explain what they're seeing, help them make decisions fast even if they're states away.
Once imaging stops being locked away and starts getting shared in real time, it's not just hospital data anymore — it's something you use.
Patient-centric imaging does not benefit patients alone.
Radiologists get secure remote access and centralized study management. No physical workstation needed. Referring physicians review imaging right there during consultations, which cuts down the administrative wait. IT departments see benefits too — centralized updates, less endpoint maintenance, infrastructure that scales more easily. Administrators notice improved referral throughput, lower costs for media production, and the sense that the organization looks more digitally mature.
Patients, meanwhile, experience direct secure access, improved comprehension, and increased confidence in clinical decisions.
True transformation occurs when infrastructure aligns the needs of all stakeholders simultaneously.
 - Created by PostDICOM.jpg)
Expanding access to imaging data requires rigorous governance. Enterprise healthcare organizations must satisfy regulatory frameworks such as the U.S. Health Insurance Portability and Accountability Act (HIPAA), regulated by the Department of Health & Human Services, and the European Union’s General Data Protection Regulation (GDPR), outlined by the European Commission.
DICOM platforms that run on the web need to encrypt data both when it's moving and when it's stored. They also need permission systems that are really detailed, tools to manage sessions, logs that track who did what, and formal agreements with vendors like BAAs.
But encryption by itself isn't enough. Organizations have to look at other risks too — what happens if someone's login gets stolen, or if patient data crosses borders where privacy laws are different, or if the whole system goes down and there's no backup plan in place. The better platforms use data replication across different locations, backups that run automatically, and failover systems so things keep working even when something breaks.
Giving patients more control is important. But it can't come at the expense of the institution's credibility. Trust gets built when there's a governance structure that's both enforceable and transparent. One you can actually audit.
Moving to web-based imaging isn't just swapping out software. It's a full IT strategy decision, one that touches infrastructure, governance, and how departments actually work together day to day.
Healthcare systems usually look at three deployment models: fully cloud-native SaaS, hybrid setups with local gateways, private cloud instances. Trade-offs show up fast—performance vs. cost, control vs. compliance overhead.
Hybrid deployments get traction at institutions with strict data residency mandates or truly massive imaging volumes. We're talking data flowing through systems at a scale that chokes infrastructure if it's not built right. But hybrid architecture introduces friction—synchronization headaches, latency spikes, the ongoing task of coordinating resources across split environments.
Cloud-native SaaS scales without the capital hit up front, which sounds great until you start mapping out vendor lock-in scenarios. You need answers on data portability. API openness. Exit clauses that don't bury you in penalties or technical debt two years down the line.
Migration planning is where theory meets reality. Legacy PACS archives hold years of imaging data. Do you move everything? Run parallel systems during transition? Phase by service line? These aren't hypothetical.
Performance can't be an afterthought. High-resolution imaging depends on efficient streaming, stable network paths. Lag during a remote consult isn't just annoying—it's a clinical risk.
Enterprise modernization is messy, and IT projects fail when departments don't align early. Pilots help. So do benchmarks that everyone agrees define success before the first server spins up.
Looking at the money side takes you past just cutting hardware.
Think about an imaging network that spans multiple sites and churns out thousands of CDs every year. When you stop making physical media, you're saving on materials, yes—but also freeing up staff time while simplifying the whole coordination mess that comes with shipping things around, which alone can consume entire afternoons depending on volume and courier reliability. What matters more is that you're not waiting on FedEx or a courier to get images where they need to go. Referrals move faster.
Here's a cost most people miss: repeat imaging. When data transfer fails or a disc shows up incomplete, patients get scanned again—money down the drain, radiation exposure on top of it. Web-based sharing that's actually secure cuts way down on duplicate scans. Budget and patients both benefit.
If you look at a three-to-five-year window, moving away from big upfront infrastructure spending toward a subscription model makes your finances way easier to predict, and knowing what you'll pay each month means you can put money into expanding clinical services instead of babysitting old equipment that breaks down exactly when you need it most.
The return on investment here builds over time, not all at once, and sometimes the biggest gains show up in places you weren't even tracking yet.
Even technically superior platforms can fail without adoption strategy.
Radiologists need to know the image quality is there, that things load fast, and that the tools actually do what they're supposed to. Referring physicians just want less hassle — if you add more login steps or make their day harder, they'll resist. IT teams want clear documentation. They want to know how it connects to what's already running.
Administrative leadership? They're looking at whether this thing scales, whether the vendor will still be around in five years, whether it keeps them compliant, and whether it fits the long game.
You can't just flip a switch. Successful modernization means you build an onboarding process, you track real metrics, you train people properly, and you keep communication open across every department involved.
The organizational shift has to happen before the technology one does.
Web-based DICOM viewers aren't just about looking at scans anymore.
AI is getting baked into radiology workflows now — automated lesion detection, tumor segmentation overlays, quantitative tracking of how things progress over time, all of it delivered right through the browser interface.
Federated healthcare networks might let imaging data stay where it is, stored locally, but still accessible across institutions through standardized APIs. Less duplication, but collaboration stays intact.
Long-term, we're probably headed toward patients controlling more of their own data. Secure imaging portals could let patients give viewing rights to specialists, insurers, or research groups without going through institutional bureaucracy every single time.
In that version of the future, imaging platforms become infrastructure nodes inside interconnected digital health ecosystems. The vendors who are actually enterprise-ready see this coming and plan for it instead of just building something that displays images.
The gap between legacy desktop viewers and web-based platforms isn't small. Architectural, really.
Desktop systems need installation, workstation setup, local maintenance. Remote access is clunky and usually depends on VPNs or secure tunnels. If you want to collaborate, you're manually sharing files.
Web-based platforms get rid of installation entirely, let you access things securely from anywhere with a browser, integrate cleanly with telemedicine, push updates from a central location, and scale elastically in cloud environments.
This isn't an upgrade. It's a different system.
What is a web-based DICOM viewer?
A browser-accessible imaging platform that enables secure visualization and interaction with DICOM studies without local installation.
Can patients securely access their imaging studies?
Yes, when platforms implement encryption, authentication controls, and regulatory safeguards.
How does web-based imaging enhance telemedicine?
It allows real-time imaging review during remote consultations, strengthening collaborative decision-making.
Is a web-based viewer the same as PACS?
No. PACS manages storage and archival functions. A DICOM viewer provides visualization and interaction capabilities.
Do cloud imaging platforms meet regulatory standards?
Enterprise-grade platforms can meet HIPAA and GDPR requirements when implemented with proper governance controls.
Patient-centric care cannot be achieved through policy alone. It requires infrastructure that enables visibility, collaboration, regulatory integrity, and scalable deployment.
Web-based DICOM viewers redefine imaging from an institutional silo to a shared clinical resource. They align radiologists, referring physicians, administrators, IT teams, and patients within a secure collaborative environment.
Platforms such as PostDICOM demonstrate that enterprise-grade security, cloud scalability, and browser accessibility can coexist without compromising diagnostic integrity.
Empowerment in modern healthcare is architectural.
And imaging modernization sits at its core.
|
Cloud PACS and Online DICOM ViewerUpload DICOM images and clinical documents to PostDICOM servers. Store, view, collaborate, and share your medical imaging files. |